Eating for Two
- Tweet
Nutrition is critical for a child's brain development
Nutrition is the single greatest environmental influence on babies in the womb and during infancy, and it remains essential throughout the first years of life.1 Prenatal malnutrition, for example, has been linked to later adverse health and cognitive outcomes.2 Likewise, malnutrition in infancy and early childhood is a key risk factor for cognitive deficits, lower academic achievement, and behavior problems.3
A proper balance of nutrients in this formative period is critical for normal brain development.4,5 Nutritional shortages can reduce cell production, affect cell size and complexity, and lead to less efficient communication between brain cells.6 Too often, the long-term results include altered cognitive functioning and deficits in learning and memory.1,7
Moreover, because of the rapid pace and lifelong effects of brain development in a child's first three years, even mild or temporary nutritional deficits can have serious and sometimes irreversible consequences.4,8,9
Good nutrition, on the other hand, promotes positive outcomes. The benefits of breastfeeding provide a good illustration of the importance of proper early nutrition. Because breast milk is the optimal diet for healthy babies in the first six months of life, exclusive breastfeeding during this period has been consistently linked to improved brain development, nutritional status, and cognitive performance.7,10-12
Without the right amounts of the right nutrients, a baby's brain cannot reach its potential.
Although genetic and disease-related factors can contribute to malnutrition, a mother's diet plays the central role in prenatal nutrition. Adequate and balanced nutritional intake during pregnancy promotes maternal and fetal health, positive birth outcomes, and child development in infancy and beyond.
Poor prenatal nutrition hinders healthy brain development and can have permanent effects on learning and behavior.1 A shortage of nutrients can pose a serious threat to the developing brain, from the earliest embryonic stages of growth to the production of synapses later in pregnancy.13
Expectant mothers often have low levels of essential brain-building nutrients.
All nutrients are important for a baby's growing brain, but some have been found to be especially critical. These include iron, zinc, choline, vitamin A, and folate (or folic acid).6
- Iron is important for brain areas involved in cognitive development,7 and recent research has also found links between iron deficiency and social and emotional outcomes.14Meat, poultry and fish are key dietary sources of iron. Others include tofu, dairy, and fortified grains.15
- Zinc can affect the brain's ability to regulate heart rate and other vital processes. Zinc deficiencies can impair the brain's function and even its structure, leading to delays in cognitive and motor development.6,16,17Eggs and shellfish are important sources of zinc. Some nuts, legumes, and red meats are also high in zinc.15
- Choline plays an essential role in early brain development, especially in areas involving learning and memory.18Milk, eggs, peanuts, and liver are among the foods richest in choline.15
- Vitamin A is closely involved in genetic processes and is required for the proper growth and functioning of brain cells.19Cod liver oil, eggs, and milk are high in vitamin A. Vegetables like carrots and spinach are also excellent sources.15
- Folate is critical for normal brain development, especially in early pregnancy. Deficiencies can cause severe abnormalities and may be associated with later social and behavioral problems.20,21Folate is provided by leafy green vegetables, citrus fruit juices, beans, and fortified grains.15
Unfortunately, women of childbearing age are likely to get too little of these critical nutrients, and many pregnant women are found to have substantial deficiencies. This is especially true among disadvantaged groups. Low-income women, minority women, and women with less than a high school education—who already face more health risks than other women—are also particularly vulnerable to iron and folate deficiencies.13,22,23
In Memphis and Shelby County, many children are affected by malnutrition beginning in the womb.
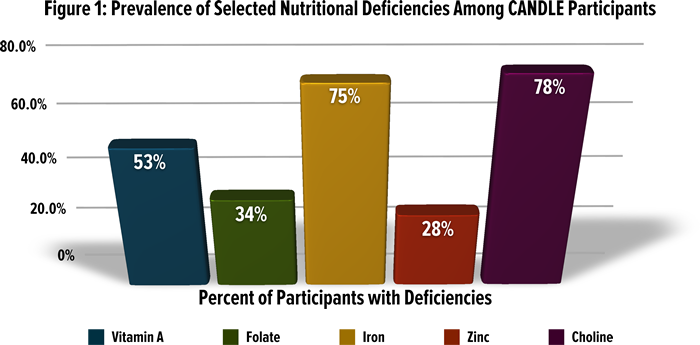
A current University of Tennessee study of Shelby County mothers-to-be shows that many of our community's children face nutritional risks even before they are born. The CANDLE study (Conditions Affecting Neurological Development and Learning in Early childhood) has collected data on the nutritional status of about 1,500 pregnant women.24 The results (Figure 1) paint a grim picture. Substantial percentages of participating women had inadequate levels of the nutrients that are most essential for healthy brain development:
- One-third of the participants do not meet the recommended levels of folate.
- Three-quarters of participants have insufficient levels of iron.
- Over one-quarter had too little zinc.
- Over half had deficiencies of vitamin A.
- Over three-quarters had insufficient choline.
These findings are consistent with national research in three important ways. First, they show that nutritional risk is not restricted to individuals suffering severe clinical malnutrition. Women eligible for the CANDLE study are considered to have relatively low-risk, healthy pregnancies. Second, shortages of the nutrients most closely linked to brain development appear to be the most common deficiencies. For many other nutrients measured by the study (not shown), only a small percentage of women were below the recommended levels.
Third, and most important, the current results underscore that nutritional risk is distressingly common. Because CANDLE participants, as a group, are roughly representative of the local population, we can reasonably assume that similar patterns would be found among expectant mothers throughout Memphis and Shelby County. Although these preliminary findings do not allow us to make specific projections or draw hard conclusions, it is clear that nutritional deficiencies are a widespread threat to our children's healthy development.
Based on age-specific Dietary Reference Intakes from:
Institute of Medicine. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids. Washington, DC: National Academies Press; 2005.
How can our community support the nutritional health of at-risk children and families?
Addressing the nutritional risks faced by mothers and babies will improve the health of our families and our community. One strategy is to increase support for existing local initiatives, such as GrowMemphis, that promote access to healthy food through community agriculture and other programs. Food insecurity—the lack of a consistent and dependable supply of healthy food—affects too many of our community's families, including many with incomes well above the official poverty line.25,26
These families frequently resort to cheaper, denser meals that are nutritionally inadequate—especially for expectant mothers eating for two. As a result, infants in food-insecure families are at high risk for nutrient deficiencies, with results that can persist even after a family's economic situation improves.27-28
Another promising area for change is suggested by a recent analysis of Memphis' food regulations. Conducted by the Harvard Law School Food Policy Initiative, the report concludes that the Memphis Food Ordinance Code is a barrier to improving access to healthy foods among at-risk families. It recommends that Memphis follow the example of other comparable cities by reforming its food codes, which currently hinder the development of alternative food delivery methods such as produce trucks, farmers markets, and urban agriculture.30
Other areas ripe for newer, more effective policies include breastfeeding promotion and nutritional screening and education among women of childbearing age. Because breastfeeding rates and nutritional knowledge tend to be lower among lower-income women, interventions in these areas could be especially beneficial for those families most at risk.31,32
Scientists are regularly making new discoveries about how nutrition affects early brain development and lifelong health. Our community can work toward a similar level of innovation by creating, supporting, and funding policies and programs that give our children a solid foundation of nutritional health, optimal brain development, and long-term well-being.
References:Morgane PJ, Mokler DJ, Galler JR. Effects of prenatal protein malnutrition on the hippocampal formation. Neuroscience and Biobehavioral Reviews. 2002; 26: 471–483.
Rizzo TA, Metzger BE, Dooley SL, Cho NH. Early malnutrition and child neurobehavioral development: insights from the Study of Children of Diabetic Mothers. Child Development. 1997; 68(1):26–38.
Wachs TD. Multiple influences on children's nutritional deficiencies: a systems perspective. Physiology and Behavior. 2008; 94: 48-60.
DeLong RG. Effects of nutrition on brain development in humans. American Journal of Clinical Nutrition. 1993; 57: 286S-290S.
Innis SM. Dietary (n-3) fatty acids and brain development. Journal of Nutrition. 2007; 137: 855–859.
Georgieff MK. Nutrition and the developing brain: nutrient priorities and measurement. American Journal of Clinical Nutrition. 2007; 85: 614S–620S.
Rao R, Georgieff MK. Iron in fetal and neonatal nutrition. Seminars in Fetal and Neonatal Medicine. 2007; 12:54–63.
Rose-Jacobs R., Black MM, Casey PH, et al. Household food insecurity: associations with at-risk infant and toddler development. Pediatrics. 2008; 121: 65-72.
Wight VR, Thampi K, Briggs J. Who are America’s poor children? Examining food insecurity among children in the United States. National Center for Children in Poverty. 2010. Available at: http://www.nccp.org/publications/pdf/text_958.pdf Accessed March 1, 2011.
Guxens M, Mendez MA, Molto-Puigmart C, et al. Breastfeeding, long-chain polyunsaturated Fatty acids in colostrum, and infant mental development. Pediatrics. 2011; 128: e880-9.
Hart S, Boylan L, Carroll S et al. Brief report: Breast-fed one-week-olds demonstrate superior neurobehavioral organization. Journal of Pediatric Psychology. 2003; 28(8): 529-534.
Tanaka K, Kon N, Ohkawa N, et al. Does breastfeeding in the neonatal period influence the cognitive function of very-low-birth-weight infants at 5 years of age? Brain and Development. 2009; 31(4): 288-293.
Rosales FJ, Reznick JS, Zeisel SH. Understanding the role of nutrition in the brain and behavioral development of toddlers and preschool children: identifying and addressing methodological barriers. Nutritional Neuroscience. 2009; 12(5): 190–202.
Lozoff B, Georgieff MK. Iron deficiency and brain development. Seminars in Pediatric Neurology. 2006; 13: 158–65.
Oregon State University, Linus Pauling Institute. Micronutrient Information Center. Available at: http://lpi.oregonstate.edu/infocenter/ Accessed on November 1, 2011
Caulfield LE, Zavaleta N, Chen P, et al. Maternal zinc supplementation during pregnancy affects autonomic function of Peruvian children assessed at 54 months of age. Journal of Nutrition. 2011; 141(2): 327-32.
Merialdi M, et al. Randomized controlled trial of prenatal zinc supplementation and the development of fetal heart rate. American Journal of Obstetrics and Gynecology. 2004; 190: 1106-1112.
Zeisel SH. Nutritional importance of choline for brain development. Journal of the American College of Nutrition. 2004; 23(6): 621S-626S.
Georgieff MK, Rao R. The role of nutrition in cognitive development. In: Nelson CA, Luciana M, eds. Handbook of Developmental Cognitive Neuroscience. Cambridge, MA: MIT Press. 2001:491–504.
Craciunescu CN, Johnson AR, Zeisel SH. Dietary choline reverses some, but not all, effects of folate deficiency on neurogenesis and apoptosis in fetal mouse brain. Journal of Nutrition. 2010; 140:1162-1166.
Schlotz W, Jones A, Phillips DI, et al. Lower maternal folate status in early pregnancy is associated with childhood hyperactivity and peer problems in offspring. Journal of Child Psychology and Psychiatry. 2010; 51(5): 594-602.
Gardiner PM, et al. The clinical content of preconception care: nutrition and dietary supplements. American Journal of Obstetrics and Gynecology. 2008; 199(Suppl): S345-56.
Scholl TO. Iron status during pregnancy: setting the stage for mother and infant. American Journal of Clinical Nutrition. 2005; 81(suppl):1218S–22S.
University of Tennessee Health Science Center. Conditions Affecting Neurological Development and Learning in Early Childhood. 2011. Unpublished raw data.
Food Research and Action Center. Food hardship: a closer look at hunger. 2010. Available at: http://frac.org/newsite/wp-content/uploads/2010/01/food_hardship_report_... Accessed March 1, 2011.
Nord M, Coleman-Jensen A, Andrews M, et al. Household food security in the United States, 2009. U.S. Department of Agriculture Economic Research Report 108. 2010. Available at: http://www.ers.usda.gov/Publications/ERR108/ Accessed March 1, 2011.
Howard LL. Does food insecurity at home affect non-cognitive performance at school? A longitudinal analysis of elementary student classroom behavior. Economics of Education Review. 2011; 30: 157–176.
Schneider JM, Fujii ML, Lamp CL, et al. The prevalence of low serum zinc and copper levels and dietary habits associated with serum zinc and copper in 12- to 36-month-old children from low-income families at risk for iron deficiency. Journal of the American Dietetic Association. 2007: 107(11): 1924-1929.
Venkateswaran R, Eyler AE, Gorenflo DW. Iron deficiency and maternal feeding practices among high-risk urban population. Journal of Health Care for the Poor and Underserved. 1998; 9(4): 381-394.
Harvard Law and Policy Clinic of Harvard Law School. Creating a more efficient and effective food safety system in Memphis and Shelby County. 2011. Available at: http://blogs.law.harvard.edu/foodpolicyinitiative/files/2011/09/Final-Me... Accessed on October 1, 2011.
American Dietetic Association. Position of the American Dietetic Association: promoting and supporting breastfeeding. Journal of the American Dietetic Association. 2005; 105(5): 810-818.
Kloeblen AS. Folate knowledge, intake from fortified grain products, and periconceptional supplementation patterns of a sample of low-income pregnant women according to the Health Belief Model. Journal of the American Dietetic Association. 1999; 99(1):33–8.